People suffer terribly from the consequences of their excess weight and many expect help from the health service. Here are some options…
A 5’2 woman who weighs 100 kg (15 st 10) has a BMI of 40 and is morbidly obese. If she manages to lose 5% of her weight, she will weigh 95 kg (14 st 13), which is a BMI of 38.6. Can anyone honestly say that this has been a sufficient treatment? To get her down in weight to the top of the normal range (BMI 25) she will have to lose 38.5 kg (approximately 6 stone).
Tell her to exercise?
The calories used in exercise will make a difference only if the patient is in calorie balance. Most overweight people are routinely eating in excess of their daily needs. Around 2,000 calories can be consumed with very little recognition that the average daily expenditure has been matched. Assuming, however unlikely, that calorie balance has been achieved, the excess weight represents 296,400 calories below the calorie balance level that will have to be used up by increased activity. At 100 calories for a mile run, the patient will simply have to run 3,000 miles (without any additional overeating).
Cut back a little to lose weight slowly?
Modest reductions in calories could theoretically result in weight loss, although the best efforts of the Swedish healthcare system could not produce any.1,2 Of course, it can’t be emphasised often enough, the modest reduction has to be from the equilibrium level, not from current intake. Standard advice has been to limit the rate of weight loss by encouraging a small calorie gap. This most often assures failure to lose substantial weight. Arguing that slow weight loss somehow results in better weight maintenance (except perhaps maintenance of the prediet weight) was convincingly demonstrated
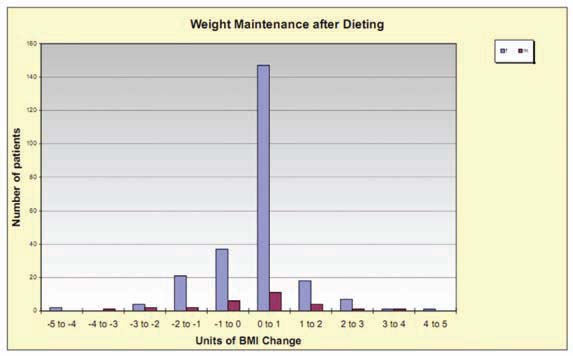
to be false as far back as 1959. Stunkard showed that regardless of the programme for weight loss, or the expertise of the clinic, after one year 95% had put back all the lost weight.3 After two years 98% and by five years virtually all of the dieters had put the weight back on.
Faster weight loss is actually better
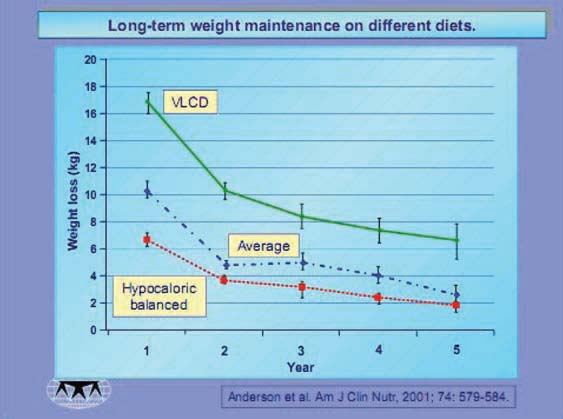
Very low calorie diet (VLCD) treatment has a well-documented, vastly better, record for weight loss and weight maintenance.4 The fallacy that reducing calorie intake sufficiently low to encourage a rapid loss of weight was harmful, resulted from the fact that the poor distribution of essential nutrients in ordinary foods makes it very difficult to create a nutrient-complete diet under conditions of food restriction. It is actually impossible to achieve an unsupplemented nutrient complete diet at intakes below 1,200 calories. When traditional food diets were attempted below 1,000 calories, dieters were put at risk. When the need for dieting was for a prolonged period, it was inevitable that various nutrient stores were depleted. The result was some sort of health compromise. The nature of the compromise and the consequences depended upon which nutrients happened to be depleted by the unique food choices of the dieter. What was required was a nutrient-complete source, which guaranteed nourishment and at the same time provided the least possible calorie levels so that a maximum rate of safe weight loss could be achieved. Liquid enteral feeds meet the nutrient criteria, but are usually designed to cause weight stability or even weight gain. These high-calorie levels are generally met by relatively high levels of fat. Simply reducing fat levels in enteral formulas solved the calorie problem. An ideal nutritional product with the absolute minimum of calories consistent with a healthy diet is achieved. The modern VLCD can be used with confidence, both in the reliability of the weight loss, and the safety of the monitored programmes. There are contraindications and medical issues that need to be understood, but under proper care the weight loss needs of seriously overweight patients can be met.
Help is available and simple to use
An expanding network of pharmacists are offering a range of treatments for weight problems. They have the training, the respect of the public, the contact hours and the desire to offer weight management as a professional service. NICE recommends that specialists be used for extended VLCD treatment.5 These pharmacists are trained and experienced specialists in the use of VLCD. Suggest a pharmacist to offer your patients real help with their excess weight. This will even reverse the ever increasing prevalence of type 2 diabetes.
References
1. Sjöström D, Peltonen M, Wedel H, Sjöström L. Differentiated long-term effects of intentional weight loss on diabetes and hypertension. Hypertension 2000;36:20-5.
2. Karlsson J, Taft C, Rydén A, Sjöström L, Sullivan M. Ten-year trends in health related quality of life after surgical and conventional treatment for sever obesity: the SOS intervention study; Int J Obesity 2007;31:1248.
3. Stunkard A, McLaren- Hume M. Results of treatment for obesity (a review of the literature and report of a series). AMA Arch Intern Med 1959;103:79-85.
4. Saris WH. Very-lowcalorie diets and sustained weight loss. Obes Res 2001;9:295S-301S.
5. MIMS. NICE publishes guidance on overweight and obesity. London: MIMS; 2007.
PDF version: 4-4-Treating-overweight-patients